When we take prescription medication, whether orally or through injection, we often don’t think too much about the instances when medications can affect your skin and what to do about it.
While these medications are designed to help your body to tackle internal conditions, they sometimes have unexpected effects on the skin, which may leave you confused about what to do.
If you’ve taken prescription medication recently and have suffered signs like itching, mild dryness, and rashes on the skin, it’s important to get medical help.
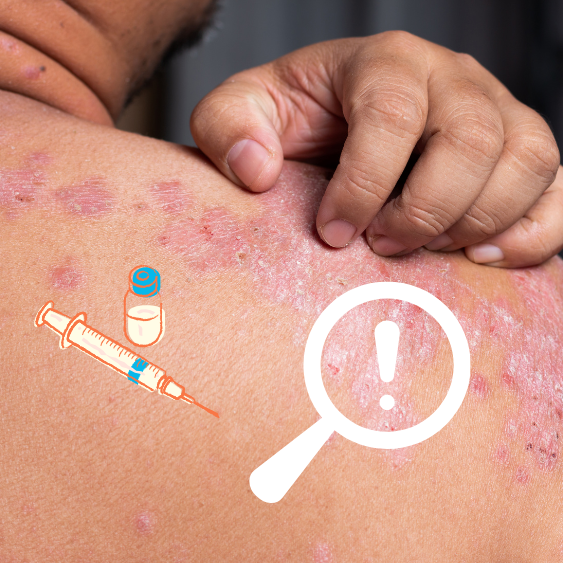
Instances When Medications Can Affect Your Skin And What To Do
Below, we’ll look at common situations in which medications can affect your skin and how you can address them.
When Medication Is Injected In The Same Area Repeatedly
You may probably know about the importance of rotating injection, but you may not know why it’s done in the first place. A doctor administering recurrent injections will advise that subsequent injections be administered at different anatomical locations for the patient’s good. Many patients think this move is taken only to reduce or avoid soreness, but there’s more to it than that.
For example, the importance of rotating GLP1 injection sites goes far beyond avoiding soreness. It’s a technique to help patients avoid impaired drug absorption, lipohypertrophy, and skin tissue inflammation.
A simple action, like rotating where you’re injected during treatment, can go a long way toward avoiding skin and other health problems and keeping you safe.
When You Take Medication That Causes Sun Sensitivity
Some medications, such as Cordarone, can cause your skin to react to sunlight, a condition known as drug-induced photosensitivity. This reaction often occurs after injecting, applying, or taking the medication by mouth, and after exposure to the sun. The drug often absorbs the UV rays from the sun and releases them into the skin, leading to cell death.
Symptoms always appear on the exposed areas after a few days and may persist for years after the medication is stopped. Apart from Cordarone medications, nonsteroidal anti-inflammatory drugs, such as tetracycline, isotretinoin, and ibuprofen, can also cause similar skin sensitivity issues.
The best way to protect your skin from drug-induced photosensitivity is to avoid sun exposure. You can stay indoors during peak sun hours or wear sunscreen daily to protect your skin from high-energy visible light, infrared radiation, UVA, and UVB.
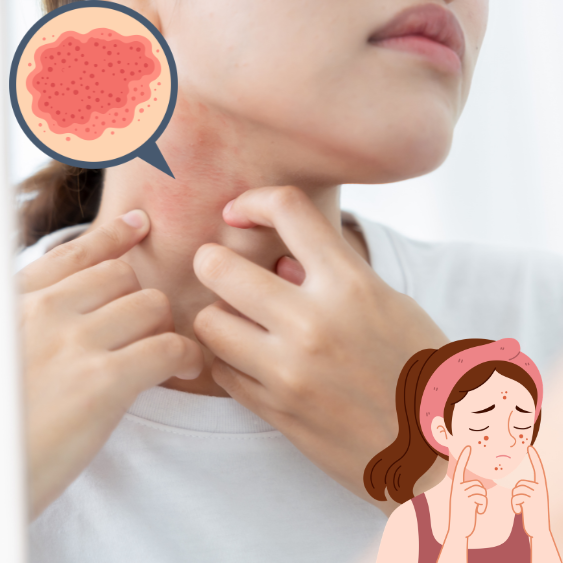
When You Take Certain Heart & Blood Pressure Medication
Some blood pressure and heart treatment medications, such as amlodipine, diltiazem, and amiodarone, can affect skin appearance when exposed to sunlight.
Amlodipine and diltiazem are classified under the drug category known as calcium channel blockers, which are known to cause hyperpigmentation on sun-exposed areas of the skin. Their effects are more enhanced in people with sensitive or fair skin.
Blood pressure medicines classified as ACE inhibitors can sometimes cause hives, itching, and angioedema, which can lead to sudden swelling under the skin. On the other hand, heart medication such as amiodarone can cause sun-exposed skin to turn blue-gray.
However, this effect on the skin is only linked to those who take heart medication for a long time. When you notice any of these symptoms, have them evaluated promptly to ensure the right solutions are administered on time.
Maintaining healthy skin isn’t always a walk in the park, but with the right approach, you can always avoid challenges, even those associated with the medications you take. If you’ve fallen victim to any of the above instances, it’s important to work closely with a doctor to ensure you get the right treatment for the predicaments.
Leave a Reply